Effective Ways to Simplify and Streamline Compliance in Healthcare Organizations
Healthcare systems today are characterized by intricate regulatory frameworks, advanced technology, interconnectedness and data sharing, evolving care delivery models, and rising healthcare expenditures. While some of these developments have the potential to enhance patient care and data management, others present compliance challenges and may foster fraudulent activities.

Healthcare organizations of all sizes face multiple challenges, including the complexity they face from multiple regulations, data protection and data security requirements, billing practices, identity theft, and cyber resilience, all of which demand robust compliance programs, advanced fraud detection, and prevention methods.
The increasing complexities of compliance also slow down the adoption and implementation of time-to-value solutions in industries such as healthcare and life sciences! As healthcare organizations and solution providers expand into new geographies, compliance challenges become even more complex.
With businesses now focusing on specializing in a specific part of activities, outsourcing critical processes and systems to vendors makes third-party compliance management a very important task. If an organization outsources work to a third party and that third party does not comply with specific regulatory and environmental standards, it could greatly impact the reputation of the outsourcing organization. With this in mind, it is critical that organizations communicate compliance and risk management standards and ensure that the vendor’s compliance management framework is aligned, effective, and agile.
How Do You Simplify and Streamline Compliance in Healthcare Organizations?
Compliance in healthcare isn’t just a virtue; it’s a requirement mandated by the Patient Protection and Affordable Care Act (ACA), making it obligatory for providers to establish and maintain a compliance plan. But is compliance merely about adhering to regulations? It extends beyond just marking the regulatory checkboxes and includes broader principles of corporate governance to ensure integrity, transparency, and trustworthiness in business operations.
Define Healthcare Compliance
Healthcare compliance involves the continuous effort to adhere to the regulatory, ethical, internal, and professional standards that pertain to a healthcare provider or organization. Compliance is also a mindset that requires a collective commitment to ethical behavior and doing what is morally right. Building a compliance culture is the foundation of a successful compliance program. It is the responsibility of the leaders of an organization to set the tone for a culture of compliance. This culture should be built on transparency, accountability, and trust. When employees understand the importance of compliance and are empowered to be a part of the solution, they are more likely to comply with regulations and policies. This culture of compliance must be reinforced at every level of the organization, from the top down, and reflected in every employee’s actions. Creating, executing, and upholding compliance programs that align with the organization’s culture and the requirements of the regulatory entities is a demanding yet indispensable obligation.
Streamline Compliance By Operationalizing It
Compliance programs created in silos and not integrated with ground business operations are ineffective. To build robust compliance programs, break down the compliance tasks into small increments and integrate them tightly with business operations. Break compliance programs down into a series of small tasks and assign them to various stakeholders. Integrate the components of compliance programs with the controls, procedures, policies, and workflows that govern business operations.
Strategically Identify and Manage Common Controls across Regulatory Frameworks
Firstly, identify the regulations that your organization needs to comply with. Once the regulations are identified, identify controls that address requirements common to multiple regulations. Centralize these controls and track the control implementation status across different frameworks, reducing the risk of overlooking or duplicating controls. Additionally, a robust compliance management platform provides better visibility and helps you create and assign controls in a systematic way to ensure effectiveness and avoid duplication. Overall, a proactive and organized approach to identifying and managing common controls enables organizations to optimize resources and enhance compliance effectiveness.
Identify Areas for Enhancing Compliance Programs through Independent Assessments
Conducting regular independent assessments allows healthcare organizations to pinpoint vulnerabilities and weaknesses in their compliance programs, ensuring a proactive approach to risk mitigation. These assessments can cover areas such as data security, privacy practices, billing procedures, and adherence to regulatory standards, providing a comprehensive view of compliance strengths and areas in need of improvement.
7 Core Elements of Strong Healthcare Compliance
The compliance program guidance created by the U.S. Department of Health and Human Services’ Office of Inspector General (OIG) recommends 7 core elements of strong healthcare compliance. To build a strong healthcare compliance program, you need to understand these core elements that serve as the foundation of compliance. These are:
Written Policies and Procedures
A comprehensive compliance program is built on written policies that outline the expectations of the organization. A good example is the code of conduct or code of ethics, which is broadly applicable to all stakeholders of the organization, including the Board of Directors. This is a key part of any compliance program, and through these policies, companies can establish their operational standards. For instance, the Code of Conduct can instruct, educate, and guide employees as well as third-parties on how to conduct themselves during business engagements.
Another vital list of documents is the one that facilitates the implementation of the compliance program. These outline the procedures for compliant action and articulate the importance of implementation and enforcement of the program.
Compliance Officer and Committee
A designated compliance officer and committee are essential for managing and overseeing the compliance program. They are responsible for the successful execution of the compliance programs. The compliance officer is responsible for monitoring, auditing, and implementing the compliance program, while the committee provides strategic guidance and ensures transparency.
Education and Training
A very essential aspect of a robust compliance program is training. To promote a culture of compliance, healthcare organizations must provide ongoing education and training for their staff. These programs should cover regulatory requirements, ethical standards, and the organization’s specific policies and procedures.
Effective Communication
Open lines of communication is essential for reporting compliance concerns. Healthcare organizations should establish mechanisms for employees to report potential violations, including anonymous reporting channels. Effective communication helps detect issues early and enables their resolution.
Monitoring and Auditing
Regular internal monitoring and auditing processes are required for identifying and rectifying compliance deficiencies. These processes allow organizations to review their practices, assess adherence to policies, and address areas of non-compliance promptly.
Response and Corrective Action
Healthcare organizations should be prepared to address any violations or issues swiftly and systematically. Establishing processes for responding to complaints, conducting investigations, and applying corrective actions is vital to maintaining compliance.
Enforcement of Standards
Enforcing compliance standards using disciplinary guidelines is important. Regardless of an individual’s position in the organization, continuous non-compliance must be met with strict consequences, such as punishments and temporary suspension. These rules help create a culture of compliance and accountability.
Best Practices for Healthcare Compliance Success
Currently, healthcare compliance places significant emphasis on program improvement and heightened efficiency. In addition to the core elements of effective healthcare compliance, as defined by OIG, here is a list of best practices that our customers have been practicing to ensure compliance success.
Risk assessment plays a crucial role
To manage the complex healthcare landscape effectively, organizations must conduct regular risk assessments. This involves identifying potential compliance risks and implementing strategies to mitigate them. It’s a proactive approach to stay ahead of evolving regulations and industry trends.
Create metrics for evaluating these program improvements
Developing measurable metrics is critical for tracking the effectiveness of compliance enhancements. Metrics can include the percentage reduction in compliance violations, improved employee training completion rates, and enhanced patient data protection measures.
These quantifiable indicators help healthcare organizations to gauge the impact of their compliance efforts and make data-driven decisions for continuous improvement.
Draw inspiration from successful practices in other organizations
Learning from the success of others allows healthcare organizations to adapt similar and proven strategies to their specific needs and challenges, encouraging innovation and efficiency. While adopting best practices from other organizations, it’s essential to customize them to align with your organization’s values, mission, and the intricacies of its healthcare environment.
Put the best practices into action and monitor the outcomes
Implementing the identified best practices is the core of healthcare compliance. This is where plans become actions and the running compliance programs become stronger. Continuous monitoring of the outcomes of the programs helps healthcare organizations remain agile, adjust strategies as needed, and demonstrate a commitment to both compliance and ongoing improvement.
Encourage whistleblowing in your compliance culture
Whistleblowers in healthcare play an important role in upholding the integrity of the industry. They are the ethical compass that exposes misconduct, instances of fraud, endangerment of patients, and regulatory violations. Recognizing their importance is crucial in maintaining a culture of transparency and accountability. Healthcare organizations and authorities must create an environment where whistleblowers are protected and encouraged to come forward, as their actions are crucial for the well-being of patients and healthcare compliance.
Leverage Three-Line Model
Collaboration between compliance officers and operational leaders in healthcare organizations is a common challenge, often stemming from a lack of awareness regarding their shared responsibilities in compliance programs. To address this issue, the Three Lines Model, developed by the Institute of Internal Auditors (IIA), can be implemented These key organizational roles can work in synergy to improve governance and risk management. This model delineates the three lines of responsibility within an organization: the first line (operational areas) identifies and mitigates risks within their departments, partnering with compliance for compliance monitoring.
The second line (Compliance, General Counsel, Risk, and Quality) facilitates training, policy creation, auditing, and monitoring for operational leaders, while the third line (independent oversight) involves internal auditors or independent consultants to assess compliance with policies, procedures, laws, and regulations. This model encourages everyone in the organization to play a role in compliance, emphasizing that it’s not solely the responsibility of the compliance department.
By combining the Three Lines Model with best practices, such as the OIG’s seven elements for compliance program effectiveness and the establishment of operational compliance committees, organizations can cultivate a collaborative approach that underlines the significance of shared responsibilities in healthcare compliance.
Major Regulations Related to Healthcare Compliance
Now, let’s look at some of the major regulations that are applicable to healthcare organizations. These regulations encompass a wide range of aspects, including patient care, billing, research, reimbursement, ACA compliance, OSHA regulations, privacy and security compliance, etc.
Here are some major regulations related to healthcare compliance:
Health Insurance Portability and Accountability Act (HIPAA)
HIPAA compliance refers to adherence to the Health Insurance Portability and Accountability Act regulations, which aim to protect sensitive patient health information. The privacy and security rules of HIPAA require healthcare organizations to implement policies, procedures, and safeguards to protect patient data, conduct risk assessments, and provide staff training on HIPAA requirements.
Example: HIPAA ensures the protection of patients’ personal health information. Healthcare providers must obtain written consent from patients before sharing their medical records with third parties, such as insurance companies or other healthcare providers.
Patient Protection and Affordable Care Act (ACA)
Commonly known as Obamacare, the ACA consists of provisions related to healthcare compliance, such as anti-fraud measures, expansion of Medicaid, and the establishment of healthcare exchanges.
Example: The ACA introduced mandatory health insurance coverage for most Americans. The ACA care provides low-income households with affordable health insurance, so they’re not forced to go without insurance if sky-high premiums exceed their budgets. The Affordable Care doesn’t allow health insurance companies to deny coverage because of pre-existing conditions or base costs on your health.
Anti-Kickback Statute
This law prohibits offering, paying, soliciting, or receiving anything of value for securing more business or referrals to federal healthcare programs. It aims to prevent fraud and abuse.
Example: A pharmaceutical company cannot provide monetary rewards or incentives to healthcare providers in exchange for prescribing their medications. Such incentives would violate the Anti-Kickback Statute.
Stark Law (Physician Self-Referral Law)
Stark Law forebids physicians from referring Medicare and Medicaid patients for certain health services to entities in which they have a financial interest. This law prevents self-referral and potential conflicts of interest.
Example: A physician cannot refer patients to a diagnostic imaging center in which they have a financial interest. This law does not allow physicians from profiting from their own referrals and ensures that referrals are based on the patient’s best interests.
Emergency Medical Treatment and Labor Act (EMTALA)
EMTALA mandates all hospitals to provide emergency medical care to all patients, regardless of their ability to pay. It prevents hospitals from dumping patients and ensures access to emergency care.
Example: EMTALA requires hospitals to provide emergency medical care to all patients, regardless of their ability to pay. If a hospital turns away an unstable patient in an emergency situation due to a lack of insurance or payment ability, it violates EMTALA.
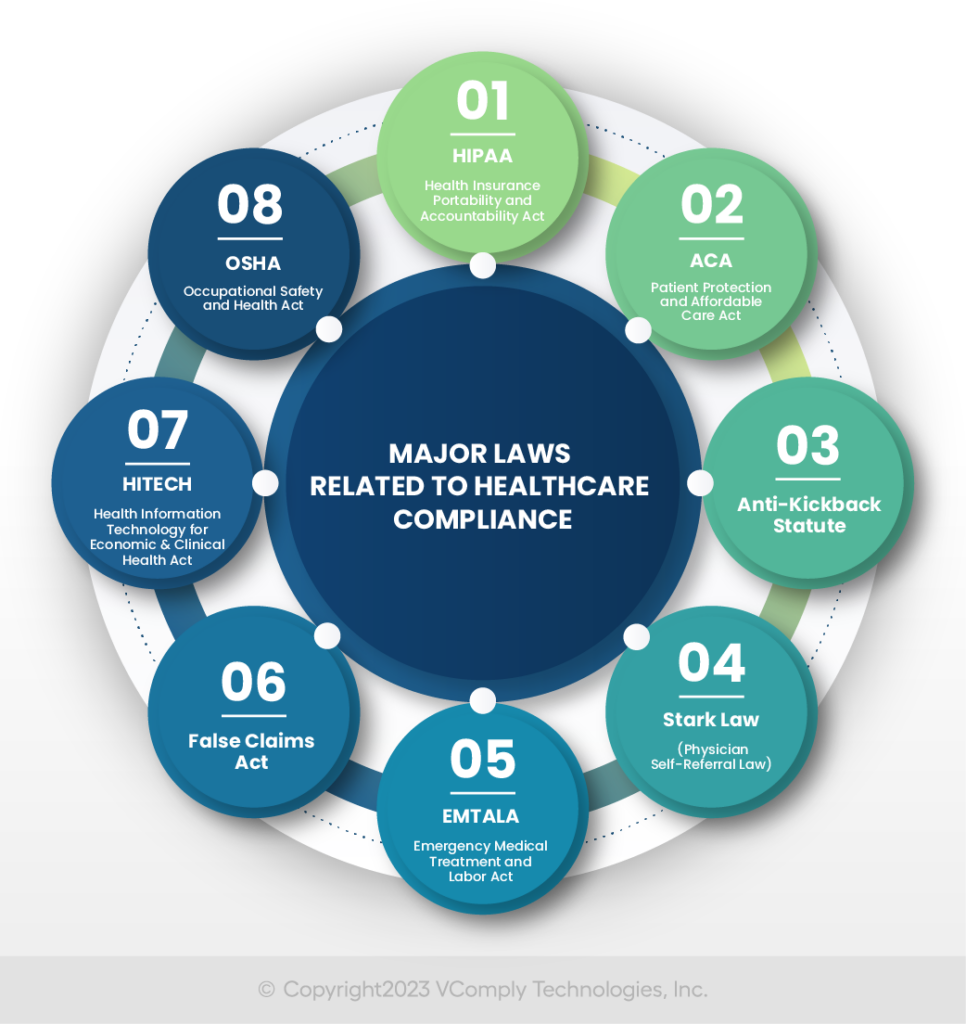
False Claims Act
This law holds accountable those who deceive government programs, including Medicare and Medicaid. It allows whistleblowers to take actions on behalf of the government.
Example: A healthcare provider who submits false claims for Medicare or Medicaid reimbursement, knowingly billing for services not provided or falsely inflating costs, could face legal action and substantial penalties under the False Claims Act.
Health Information Technology for Economic and Clinical Health Act (HITECH)
HITECH complements HIPAA and set stricter standards for electronic health records (EHR). It also enforces penalties for data breaches and violations of patient privacy.
Example: If a healthcare organization experiences a data breach that affects more than 500 individuals, they must report it to the Department of Health and Human Services (HHS) and the affected individuals.
Occupational Safety and Health Act (OSHA)
OSHA sets workplace safety and health standards, applicable to healthcare settings, to protect employees from hazards and ensure safe patient care environments.
Example: OSHA includes regulations on the use of personal protective equipment (PPE) to protect healthcare workers from exposure to infectious diseases, such as COVID-19.
These major regulations, among others, collectively create a framework that healthcare organizations and professionals must adhere in order to ensure the highest standards of care and compliance. Implement automation and workflows to manage multiple regulatory frameworks, automate tasks, and minimize errors, leading to increased efficiency and cost savings. Establish controls, notify stakeholders of their due obligations, and ensure adherence to the standards.
VComply Helps Organizations Across the Healthcare Industry
VComply is an integrated compliance and risk software solution that helps organizations manage compliance frameworks and implement compliance programs efficiently. The platform lets you create controls, define roles, and assign them to various stakeholders. It tracks and monitors your compliance controls but also keeps a tab on the organizational risks and helps mitigate them on time proactively. VComply offers many benefits — you can automate workflows, do follow-ups, and report obligations and issues, so you don’t miss a deadline. VComply provides a central system of record for compliance with easy accessibility. The tool promotes collaboration and holds everyone accountable for their respective roles in adhering to the compliance and risk management framework.
VComply also lets you create various units and departments on the platform, and its workflows support seamless collaboration between these departments. It simplifies evidence management and provides a systematic approach to uploading and centralizing evidence. Using VComply’s compliance assessment feature, you can analyze the gap in your compliance processes, and provide a systematic approach to evaluating adherence to regulations. The platform’s dashboards and reports provide a 360 degree view of compliance trends, compliance activities, and status. The due diligence score helps you improve the accountability of the stakeholders and ensures that the responsibilities are met. You can stay informed on compliance status and updates with VComply’s alerts and notifications, and ensure seamless collaboration and timely response. With its multifaceted capabilities, VComply helps organizations simplify and streamline their compliance processes, manage risks, and ensure adherence to regulatory standards.
